Lotrisone
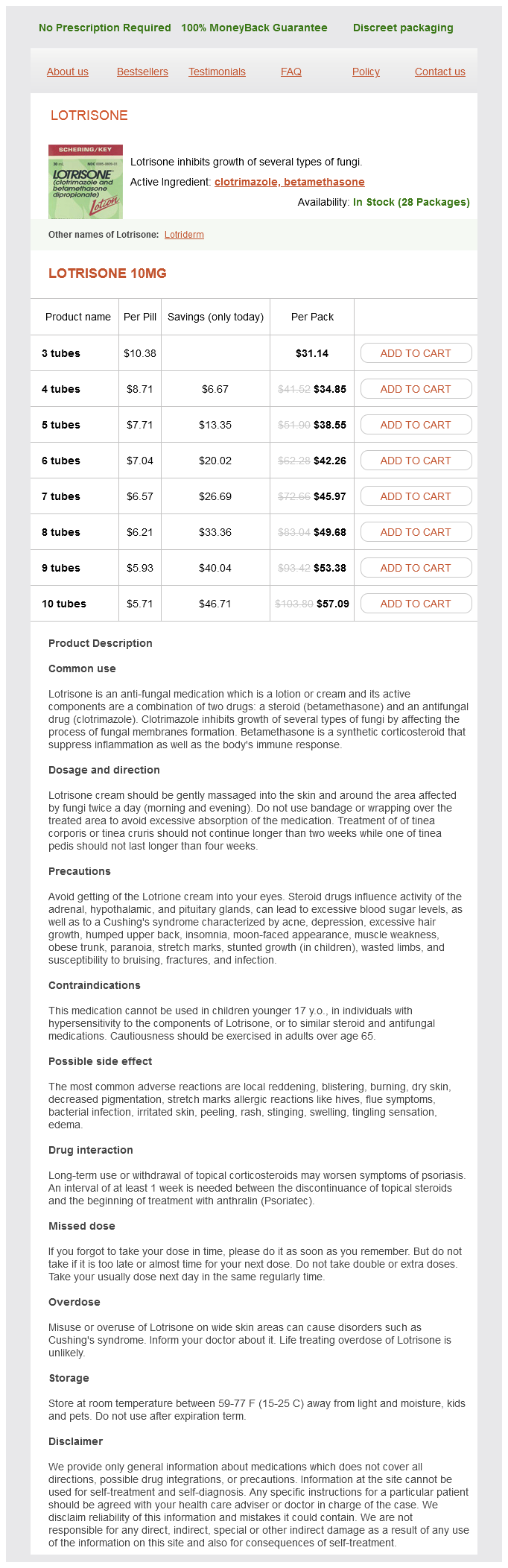
Lotrisone 10mg
- 3 tubes - $31.14
- 4 tubes - $34.85
- 5 tubes - $38.55
- 6 tubes - $42.26
- 7 tubes - $45.97
- 8 tubes - $49.68
- 9 tubes - $53.38
- 10 tubes - $57.09
Lotrisone dosages: 10 mg
Lotrisone packs: 3 tubes, 4 tubes, 5 tubes, 6 tubes, 7 tubes, 8 tubes, 9 tubes, 10 tubes
In stock: 811
Only $6.07 per item
Description
Aspirate all the blood from under the left cupola 4 n Make sure the duodenal stump is safely closed fungus gnats biological control buy generic lotrisone 10 mg on line. If so, does this replace careful technique and should you therefore re-close the duodenum or reinforce the closure Alcohol causes acute gastritis with bleeding from this or, following retching, from Mallory-Weiss tears around the cardia. Draw the greater omentum, transverse colon and mesocolon through to the right so there is no weight of colon resting on the anastomosis. Check the haemoglobin and haematocrit, and exclude clotting deficiencies if suspected. Remember that mortality is highest among the over-60s, those with massive haemorrhage and shock, and those with serious associated disease. Do not embark on surgery for upper gastrointestinal bleeding alone if there is someone more experienced available. Access Make a generous upper abdominal midline incision skirting the umbilicus, 2025 cm long. Look for continuing bleeding and the presence of visible vessels which indicate that the bleeding is likely to continue or recur. Even if you cannot identify the source you can usually exonerate particular areas, for example excluding oesophageal varices. Haemostatic substances can be injected in association with local application of heat. Assess 1 n As the abdomen is opened, blood which appears bluish through the bowel wall may be seen in the small or large bowel. Dilated and congested veins on the viscera with a stiff cirrhotic liver make portal venous hypertension obvious. Therefore carry out a thorough check of the lower oesophagus, stomach and duodenum, remembering that there may be an unsuspected lesion in the small or large bowel. It may be valuable first to have a large-bore gastric tube passed so that the stomach can be washed out if it contains blood or retained food. In appropriate circumstances the radiologist may be able to embolize the feeding vessel. This makes it dangerous to defer operation if bleeding is serious and not controllable. Make an incision through the anterior gastric wall midway between the greater and lesser curves in the distal stomach, carrying this through the pylorus in to the anterior duodenal wall for 23 cm if necessary. Insert large-bladed retractors for your assistants, have the light adjusted to shine in to the stomach and carefully examine the interior of the stomach and if necessary the duodenal bulb, seeking the cause of bleeding. Sometimes the gastric wall can be evaginated through the gastric wound to allow close inspection. If the pylorus has not been incised it is often possible to insert thin-bladed retractors through it to view the duodenal bulb, or a flexible cystoscope may be passed, offering excellent views of the bulb. If there is no active bleeding and no cause is found, close the abdomen and determine to repeat the endoscopy at the first sign of re-bleeding, followed if necessary by other methods of detection and isolation of bleeding sites. Action 1 n Bleeding duodenal ulcer is preferably treated at present by pyloroplasty or duodenotomy, and suture of the bleeding vessels.
Ivy Gourd. Lotrisone.
- Are there any interactions with medications?
- Dosing considerations for Ivy Gourd.
- Are there safety concerns?
- What is Ivy Gourd?
- How does Ivy Gourd work?
- Diabetes, gonorrhea, constipation, and skin abscesses.
Source: http://www.rxlist.com/script/main/art.asp?articlekey=97050
However anti yeast antifungal shampoo buy discount lotrisone 10 mg line, the operative mortality is twice that following vagotomy with under-running of the bleeding vessel, and the side-effects and late sequelae may be more severe. Consequently, the most frequently performed procedure is vagotomy with pylorotomy following under-running of the ulcer with non-absorbable stitches. Erosive bleeding rarely demands operation but multiple haemorrhages can be dealt with only by excision of the affected gastric wall by gastrectomy. Polya gastrectomy allows the creation of a stoma the full width of the stomach, which is thus unlikely to become obstructed if the tumour recurs. Since the duodenum is closed, this isolates it from distal spread as may occur if gastroduodenal anastomosis is used. The preferred method of resecting distal gastric carcinoma is by radical subtotal gastrectomy with Polya or Roux-en-Y reconstruction. From time to time it offers a convenient way of fashioning the anastomosis for benign disease. It cannot be used conveniently for high gastroenterostomy to relieve malignant distal gastric obstruction. Identify the middle colic vessels and make a conveniently placed vertical hole through the mesocolon to one or other side of them, 57 cm long. If the operation is for carcinoma, start in the pelvis and lower abdomen, para-aortic region and root of the mesentery, proceeding to the liver before touching the stomach in order to avoid carrying malignant cells around the peritoneal cavity. The size of the anastomosis between the proximal gastric stump and the duodenum is restricted to the diameter of the duodenal lumen and if the cancer recurs there is a risk of anastomotic obstruction. If necessary, open the lesser omentum or gastrocolic omentum to examine the posterior wall of the stomach and contents of the lesser sac, including the glands around the coeliac axis and along the superior border of the pancreas. Resect 1 n Make a hole in an avascular area of the gastrocolic omentum to the left of the gastroepiploic vascular arch. Identify the posterior gastric wall and separate it from the pancreas and transverse mesocolon. Insert a second invaginating seromuscular suture to cover the first stitch line or insert a purse-string suture and invaginate the first suture line as it is tightened and tied. If possible, insert a third stitch that picks up and draws together the ligated right gastric and right gastroepiploic vessel stumps, the anterior duodenal wall and the peritoneum over the head of the pancreas. To the right, divide and ligate the main right gastroepiploic vessels as they lie near the inferior border of the pylorus. The separation of this vascular tissue can be accomplished rapidly using ultrasonic. Harmonic Scalpel, Ethicon Endosurgery) or tissue response generator (Ligasure, Covidien) dissection. When Polya gastrectomy was the standard operation for duodenal ulcer, a two-thirds gastrectomy was usually carried out. Isolate the vessels from the lesser curve of the stomach, doubly clamp, divide and ligate them.
Specifications/Details
Pancreatic injury following laparoscopic splenectomy resulting in pancreatitis and pancreatic fistula occurs in 13% of cases anti fungal bacterial cream lotrisone 10 mg order without a prescription. A colonic or stomach injury should be closed using interrupted seromuscular absorbable sutures. Undetected pancreatic injury may later present as pancreatic ascites, a subphrenic collection or pancreatic fistula. We recommend routine subcutaneous heparin prophylaxis and compression stockings in all patients. There are fewer respiratory complications after laparoscopic splenectomy with early mobilization and discharge on the second or third postoperative day. Chest infection may result from splinting of the left diaphragm causing atelectasis. Subphrenic abscess has been reported in 4% of patients after open splenectomy for all indications in a large series. This complication is less common after laparoscopic splenectomy and in the absence of gastrointestinal trauma. A subphrenic collection can usually be drained percutaneously with antibiotic cover but may occasionally require a laparotomy. The ability to identify accessory spleens using laparoscopic techniques is in question. The initial step during laparoscopic splenectomy is a systematic exploration for accessory splenic tissue. When identified, they are immediately removed because they may be easily lost during the dissection. Small splenic tears may be controlled with compression by surrounding tissues and haemostatic diathermy. However, the spleen is an end organ and the quickest way to get control of a difficult situation is to mobilize the spleen and get control of the hilar vessels. Once the spleen has been mobilized on to the abdominal wall, a soft bowel clamp is applied across the splenic hilum. This will control the situation and allows the anaesthetist time to resuscitate the patient before completing the operation. When the patient is stabilized, the soft bowel clamp can be sequentially removed to ligate the hilar vessels and to make sure that the tail of the pancreas is not damaged. Postoperative bleeding is suspected if the patient becomes unstable or a drain, if used, produces a large amount of fresh blood. If the patient is stable, re-laparoscopy can be undertaken to look for the site of bleeding. If the patient is unstable, urgent laparotomy is preferred to control the bleeding site. The risk is higher in young children (410%) and after splenectomy for haematological disease, but fatal cases have also been reported in adults. Though long-term oral antibiotic prophylaxis is controversial, all patients should be thoroughly counselled to seek 8 n Accessory spleens are noted in 1530% of patients and account 9 n Other sporadic complications include trocar site hernias, wound infection and ileus.
Syndromes
- You are nauseated
- Anxiety attack
- Did the pain rapidly get worse?
- The bladder wall changes. The elastic tissue becomes tough and the bladder becomes less stretchy. The bladder cannot hold as much urine as before.
- Death
- Constipation
- May feel dull, tight, or like a band around the head
- If you have diabetes, heart disease, or other medical conditions, your surgeon will ask you to see the doctor who treats you for these conditions.
Related Products
Usage: q.h.
Additional information:
9 of 10
Votes: 162 votes
Total customer reviews: 162
Customer Reviews
Falk, 40 years: Central haematomas that are to the left of the midline are best explored by rotating the left-sided abdominal viscera to the midline. Above the pylorus, identify the right gastric vessels, trace the arteries up to their origin 14 n Extend the radial cut in the diaphragm to the crura.
Volkar, 54 years: Change of direction may be achieved by angulation of the distal end, up/down or left/right. Access Operations for chronic pancreatitis require generous access to the upper abdomen.
Jarock, 41 years: Radiotherapy has been used instead of surgery in some series and Pearson reported results as good as those obtained with surgery, especially for mid- and upper oesophageal tumours. In operations for carcinoma of the right colon it is not necessary to resect more than a few centimetres of terminal ileum.
Dargoth, 29 years: We always place two ties on the proximal cut stump or transfix it with an arterial suture. The vaccine is not expected to be effective in women already persistently infected with the virus.
Barrack, 65 years: Insert a bunched-up piece of polypropylene mesh through the small defect in to the extra-peritoneal space and secure it with a few sutures across the open defect. The esophagus is dilated and the scope passes through the gastroesophageal junction with some gentle pressure.
Karrypto, 21 years: Check 1 n Carefully inspect the cut surface to ensure haemostasis and no 2 n Carefully inspect the liver hilum to ensure that no major structures have been damaged. If no bowel is being resected or anastomosed, do not open the bowel to attempt decompression, 2.
Contact
0673406227
dppsmyanmar@gmail.com